“Your thoughts are not just thoughts. They are biological signals your immune system is receiving and acting on right now. That is not a metaphor. That is science.”
Josh Trent
There is a field of science that has been quietly reshaping everything we understand about how the human body works. It is called psychoneuroimmunology, and if you have ever wondered why a brutal season of stress seemed to follow you straight into a sinus infection, or why your body tends to fall apart right after a major deadline finally passes, this is the science that has your answer.
Psychoneuroimmunology is not a fringe theory invented on a wellness podcast. It is a rigorous, peer reviewed discipline sitting at the exact intersection of psychology, neuroscience, and immunology. It shows us, in exquisitely clear biological detail, that your thoughts, your emotions, your unresolved grief, and your daily stress load are not metaphors for illness. They are actual biological signals your immune system receives and responds to in real time.
I have been exploring the mind body connection through the Wellness + Wisdom Podcast for over a decade, and of all the fields I have studied, psychoneuroimmunology is the one that most completely validates what healers, indigenous grandmothers, and contemplative traditions have always known: how you feel matters to how your body functions, and these two realities are not separate systems. They are one living whole.
This article is your guided tour through that science. We are going to look at what psychoneuroimmunology actually is, how the stress and immune system relationship works at the cellular level, what research tells us about how stress causes disease, and most importantly, what you can do about all of it. Because the science does not just explain the problem. It illuminates the path toward healing.
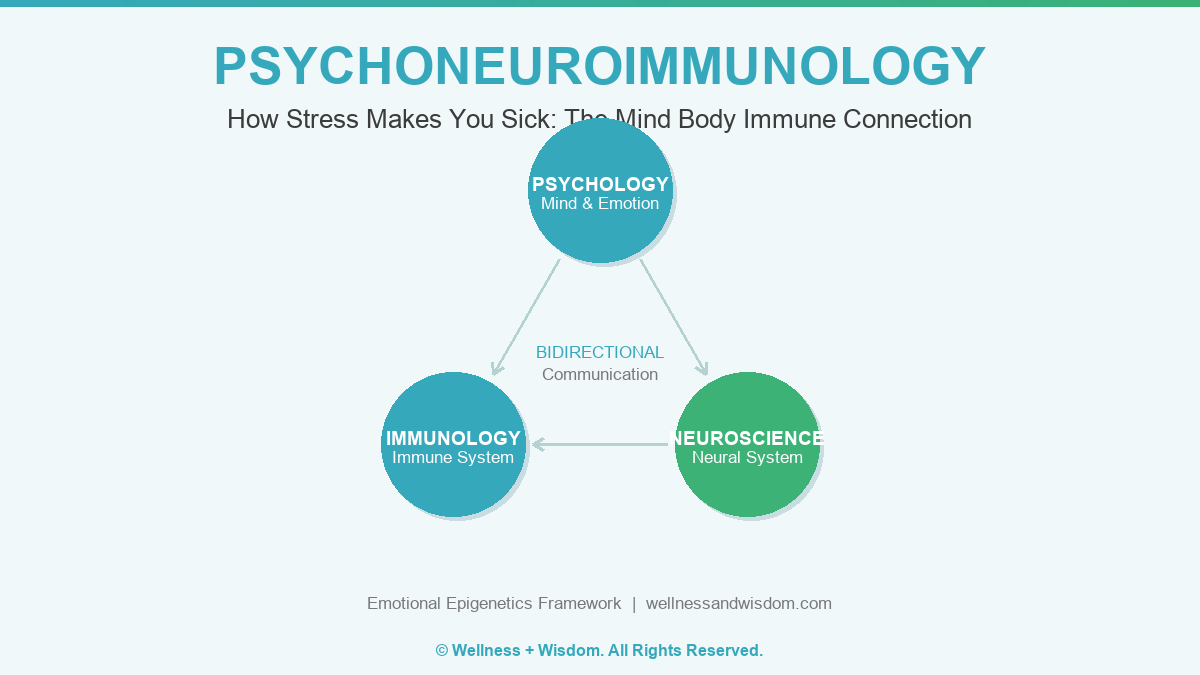
What Is Psychoneuroimmunology? The Field That Changes Everything
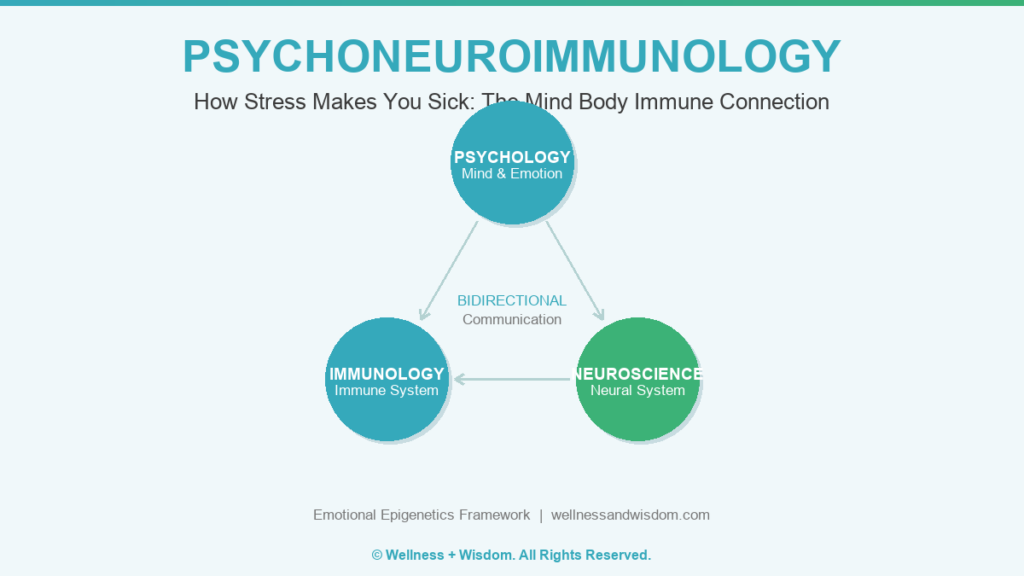
The word itself sounds designed to intimidate you. Break it down and it becomes simple. Psycho refers to the mind and psychological experience. Neuro refers to the neural system and its intricate signaling architecture. Immuno refers to the immune system, your body's defense and surveillance network. And ology means the scientific study of something.
Put them together and psychoneuroimmunology is the scientific study of how the mind, the neural system, and the immune system communicate with each other in real time, and what that communication means for your health. It is the formal science of the mind body connection, and it is far more advanced and established than most doctors will ever mention to you.
The field was formally born in 1975 when psychologist Robert Ader and immunologist Nicholas Cohen conducted an experiment that stunned the scientific community. They discovered that the immune system could be classically conditioned using behavioral cues, the same way Pavlov had conditioned dogs to salivate at a bell. This was a seismic discovery because the prevailing assumption at the time was that the immune system operated in complete autonomy, totally separate from the brain and the mind. Ader and Cohen proved that assumption completely wrong.
What they showed was that the immune system is not a closed, self-contained defense department. It is a bidirectional communication partner with the brain and neural system. Every psychological experience you have, from the momentary frustration of traffic to the years-long grief of losing someone you love, sends signals that reach your immune cells and changes how they behave.
Since that foundational discovery, psychoneuroimmunology has grown into one of the most generative research fields in modern science. The Psychoneuroimmunology Research Society, which holds its 2026 annual meeting in New Orleans under the theme “Modifiable Risk Factors Across the Lifespan,” now brings together hundreds of researchers from fields as diverse as oncology, psychiatry, molecular biology, and behavioral medicine. The science is robust. The evidence is clear. And yet your primary care physician almost certainly has not told you about it.
Why not? Because medical training still tends to partition the body into separate specialties. The cardiologist sees the heart. The neurologist sees the brain. The immunologist sees the immune system. The psychologist sees the mind. And rarely does any single practitioner ask what happens at the borders between all of those systems. Psychoneuroimmunology asks exactly that question, and its answers change everything.
Your Body's Three Way Conversation: Psychology, Neuroscience, and Immunity
To understand psychoneuroimmunology is to understand that your body is conducting an extraordinarily complex three way conversation at every moment of every day, whether you are consciously participating in it or not. The three parties in this conversation are your psychological experience (thoughts, emotions, beliefs, memories, perceptions), your neural system (brain, spinal cord, autonomic pathways, and peripheral nerves), and your immune system (white blood cells, antibodies, cytokines, lymph nodes, the spleen, and the gut-associated lymphoid tissue).
For most of the twentieth century, scientists treated these systems as separate departments with separate budgets, separate languages, and separate research silos. What psychoneuroimmunology revealed is that these three systems are not just vaguely connected in some poetic, feel-good way. They share molecular messengers. They carry each other's receptors. They change each other's behavior in response to information that flows in both directions.
Here is the core mechanism. Your neural system and your immune system speak the same molecular language. Immune cells carry receptors for neurotransmitters including norepinephrine, acetylcholine, and serotonin. They also carry receptors for neuropeptides like substance P and endorphins. When your brain activates those signaling pathways, immune cells respond directly. Conversely, when your immune system activates during an infection or inflammatory event, it releases cytokines that travel to the brain and alter mood, cognition, motivation, and even social behavior.
This is why you feel depressed, foggy, and socially withdrawn when you are sick. That constellation of feelings is not a side effect. It is an actively orchestrated immune to brain signal called sickness behavior, a coordinated biological strategy designed to make you rest, withdraw from social risk, and redirect energy toward healing. It is the immune system literally commanding the brain to slow down and cooperate with recovery.
This is the Wellness Pentagon in action at the biological level. Your physical, mental, emotional, spiritual, and even financial experiences are not siloed events happening in separate compartments. They are woven into a unified biological web, and psychoneuroimmunology is the science that maps the threads.
The implication for your health is enormous. If every psychological experience sends biological signals to your immune system, then the quality of your inner life is not just a matter of personal preference or spiritual virtue. It is a direct input into your physical health, your disease susceptibility, your recovery speed, and your longevity. What you carry emotionally, you carry biologically.
The HPA Axis: Your Stress Escalation System Explained
To fully appreciate the psychoneuroimmunology of stress, you need to understand the hypothalamic pituitary adrenal axis, commonly called the HPA axis. This is the master neuroendocrine system through which your brain translates psychological stress into physical hormonal signals, and it is the primary pathway through which chronic stress suppresses and dysregulates your immune function.
Here is how it works. When your brain perceives a stressor, the hypothalamus (a small but mighty region at the base of the brain) releases a hormone called corticotropin releasing hormone (CRH). That CRH travels a short distance to the pituitary gland, which responds by releasing adrenocorticotropic hormone (ACTH) into the bloodstream. ACTH then travels to the adrenal glands, which sit on top of your kidneys, and instructs them to release cortisol.
Cortisol is the body's primary stress hormone, and in acute, short term situations, it is genuinely helpful. It mobilizes energy, sharpens focus, dials down digestion and reproduction to redirect resources toward the perceived threat, and temporarily modulates immune activity to prioritize immediate survival. This is the cascade that kept your ancestors alive when a predator appeared. It is brilliant, elegant, and beautifully designed.
The problem is that this system was designed for acute, short term threats with a clear resolution. It was not designed for chronic, relentless, ambiguous modern stressors like financial pressure, relationship tension, work overload, loneliness, social comparison, news cycles, and the thousand small indignities of a dysregulated digital life. When the HPA axis is activated repeatedly without resolution, the result is not the brilliant short term survival response. The result is sustained cortisol elevation, immune dysregulation, and eventually disease.
A landmark 2025 review published in the International Journal of Molecular Sciences and indexed on PubMed (PMID 41155288) synthesized the evidence on chronic stress and autoimmunity through this exact lens. The researchers found that chronic HPA axis activation leads to glucocorticoid receptor resistance, a state in which the body's cells literally stop listening to cortisol's antiinflammatory signals even as cortisol levels remain elevated. The result is a paradoxical proinflammatory state: high cortisol with impaired cortisol response, and an immune system that has essentially gone rogue.
This is the HPA axis in failure mode. And it is, according to the evidence in psychoneuroimmunology, extraordinarily common in modern adults who have not learned to resolve their stress at the source.
Stress and the Immune System: What the Research Actually Shows
The relationship between stress and the immune system is not theoretical. It has been documented in controlled studies for decades, and the findings are striking enough that they deserve to be taught in every health education class on the planet.
The most elegant demonstration came in 1991, when psychologists Sheldon Cohen, David Tyrrell, and Andrew Smith published a landmark study in the New England Journal of Medicine. They recruited 154 healthy adult volunteers and assessed their psychological stress levels using validated scales. Then they exposed every participant to one of five different cold viruses via nasal drops. What they found was stunning. Participants with higher psychological stress scores were not just slightly more likely to develop a cold. They were significantly more susceptible across every stress measure and every virus strain. The researchers controlled for other factors including age, sex, education, allergies, weight, and health habits. The stress and immune system relationship held firm.
The conclusion was direct: psychological stress suppresses immune function in a dose-dependent way, meaning the more stress, the more immune suppression. This study, available on PubMed (PMID 1713648), is considered a foundational pillar of psychoneuroimmunology research.
The mechanisms behind that finding have since been mapped in considerable detail. Here is what happens to your immune system under sustained psychological stress:
- Natural killer (NK) cell activity decreases. NK cells are your immune system's first responders against viral infections and cancer cells. Chronic stress consistently reduces their number and activity.
- T cell proliferation slows. T cells are critical adaptive immune cells that coordinate targeted responses to specific pathogens. Stress hormones suppress their ability to multiply and respond effectively.
- Vaccine efficacy decreases. Research consistently shows that stressed individuals mount weaker antibody responses to vaccines, meaning the immune system is literally less capable of learning from protective exposures.
- Wound healing slows. Stressed individuals heal more slowly after injury or surgery, a finding that has significant implications for surgical outcomes and recovery from illness.
- Latent viruses reactivate. Herpes simplex, Epstein-Barr, and other latent viruses that healthy immune surveillance keeps dormant will often reactivate during periods of chronic stress, a clear indicator of immune suppression.
A 2025 empirical study examining the psychoneuroimmunology axis in firefighter recruits, published in the International Journal of Molecular Sciences and available on PubMed Central, found that even acute occupational stress induces measurable changes in key autoimmune biomarkers including C-reactive protein (CRP), complement factor C4, and pigment epithelium derived factor (PEDF). This is important because it shows that the stress and immune system conversation is not limited to years of chronic tension. It begins immediately, with the first stress signal, and it leaves measurable biological fingerprints.
What this means for you is simple and profound: the stress you are carrying right now is changing your immune response right now. Not metaphorically. Biochemically.
How Psychoneuroimmunology Explains How Stress Causes Disease
Understanding how stress causes disease requires understanding one word: inflammation. Not the acute, productive inflammation that rushes blood and immune cells to a cut on your finger or a twisted ankle. That kind of inflammation is a feature, not a bug. The dangerous kind is chronic, low grade systemic inflammation, a persistent state of immune activation that smolders quietly in the background, damaging tissues and organs over months and years.
Psychoneuroimmunology has identified the precise molecular mechanisms through which chronic psychological stress drives this smoldering inflammation. The primary actors are a class of immune signaling molecules called cytokines. In a healthy, well-regulated immune response, cytokines coordinate the attack on pathogens and then subside when the threat is neutralized. But under chronic stress, the regulation of cytokine production breaks down, and several proinflammatory cytokines begin to circulate persistently at elevated levels.
The three most studied proinflammatory cytokines in psychoneuroimmunology research are interleukin-6 (IL-6), tumor necrosis factor alpha (TNF-alpha), and interleukin-17 (IL-17). All three have been linked to the development and progression of serious chronic diseases when chronically elevated. The evidence base includes cardiovascular disease, type 2 diabetes, depression, certain cancers, neurodegenerative conditions, and a growing list of autoimmune disorders.
The 2025 autoimmunity review on PubMed (PMID 41155288) is particularly instructive here. The researchers documented that chronic stress and the resulting HPA axis dysregulation create a specific immunological shift: the balance tips away from regulatory, antiinflammatory immune activity and toward a proinflammatory, potentially autoimmune state. This shift has been mechanistically linked to conditions including systemic lupus erythematosus, rheumatoid arthritis, and multiple sclerosis.
To be clear about what this means: the research is showing that the emotional experience of chronic stress, the anxiety that keeps you up at night, the grief you have not been able to move through, the anger that has nowhere to go, is not just psychologically uncomfortable. It is an active driver of immune dysregulation at the molecular level. Psychoneuroimmunology provides the biological evidence for what your body has been trying to tell you all along.
The Autoimmune Connection
Autoimmune conditions represent one of the most striking expressions of stress-driven immune dysregulation that psychoneuroimmunology has helped illuminate. When the immune system is persistently activated by chronic stress and the HPA axis is dysregulated, the distinction between self and non-self, the immune system's fundamental organizing principle, can begin to blur. The immune system starts targeting the body's own tissues.
This is not random. There is a clear biological logic. When glucocorticoid receptor resistance develops under chronic stress, the immune system loses its primary regulatory brake. The result is cytokine imbalance: elevated IL-6, TNF-alpha, and IL-17 with depleted levels of the antiinflammatory cytokine IL-10. That specific imbalance is characteristic of active autoimmune states. Chronic stress does not merely correlate with autoimmune disease flares. According to the current evidence in psychoneuroimmunology, it may contribute to their initiation and perpetuation through precisely these mechanisms.
If you are living with an autoimmune condition and your doctor has never mentioned the word psychoneuroimmunology, you are not alone. But you deserve to have this part of the picture. The 800+ latest episodes of the Wellness + Wisdom Podcast include numerous conversations with researchers and clinicians at the leading edge of mind body medicine, and this theme appears again and again: addressing the stress and emotional roots of immune dysregulation is not optional support care. It is core medicine.
Emotional Epigenetics and Psychoneuroimmunology: The Link Your Doctor Missed
Here is where the science gets genuinely breathtaking, and where my own framework of Emotional Epigenetics intersects with psychoneuroimmunology in a way that opens entirely new doors for healing.
Psychoneuroimmunology tells us that your current psychological experience sends real-time signals to your immune system. Emotional Epigenetics extends that insight in two critical directions: backward and forward through generations. Backward, because the stress patterns, emotional suppression habits, and fear-based neural system wiring you carry today may not have originated with you. They may have been shaped by the unresolved stress responses of your parents, grandparents, and even earlier ancestors, transmitted through epigenetic mechanisms that alter gene expression without changing the DNA sequence itself. Forward, because the way you resolve, or fail to resolve, your own stress patterns will leave epigenetic imprints that influence your children and grandchildren.
This is not poetic language. The science is specific. Epigenetic research has shown that stress-responsive genes, including the genes that regulate cortisol production, cytokine expression, and immune cell behavior, can be methylated (silenced) or demethylated (activated) by environmental and emotional experiences. These methylation patterns can be inherited across generations. The famous research of Rachel Yehuda on Holocaust survivors and their descendants documented persistent cortisol dysregulation and altered FKBP5 gene methylation in children who had not themselves experienced trauma. Psychoneuroimmunology and epigenetics are telling the same story from different angles.
What this means for you is liberating, not deterministic. It means that healing your relationship to stress, learning to complete the stress response cycle, building genuine emotional regulation capacity, and creating conditions for authentic joy, is not just a personal wellness preference. It is an act of biological inheritance. You are literally changing the epigenetic signals your children will receive. You are rewriting the biological program that psychoneuroimmunology says influences immune function across the lifespan.
The three pillars of Emotional Epigenetics are emotional patterns (bioenergetic memory, inherited emotional responses, trauma imprints), unconscious beliefs (inherited mindset, limiting beliefs installed before age seven), and environment (the epigenetic signals sent by your lifestyle, relationships, and daily emotional state). Every one of these pillars has a direct channel into the psychoneuroimmunology network. Your emotional patterns influence your neural system activation. Your unconscious beliefs shape your cortisol response. Your environment determines the cytokine milieu your immune cells are swimming in.
This is why I describe healing through the lens of Emotional Epigenetics as a complete act, not just a personal one. Your healing ripples forward in time in ways that are measurable, biological, and real.
Mind Body Connection Science: Moving Beyond Theory Into Liberation
The mind body connection is no longer a hypothesis. It is a map with extraordinary precision, and psychoneuroimmunology is the cartography. But knowing the map is not the same as walking the terrain. The question that matters most, after understanding all of this science, is what you actually do with it in your life, your body, your relationships, and your daily experience.
One of the most important findings in mind body connection science is that the relationship between psychological experience and immune function is not just a one way street running from mind to body. It runs in both directions with equal force, and this bidirectionality is your leverage point.
Just as chronic stress and unresolved emotional pain suppress and dysregulate immune function, practices that generate genuine states of safety, connection, and joy can restore and enhance it. This is not wishful thinking. The research is clear. A 2020 study by Chaix and colleagues published in Frontiers in Psychology documented that long term meditation practice produces measurable epigenetic changes in genes involved in inflammatory regulation, including reduced methylation of genes associated with proinflammatory responses. The mind, cultivated deliberately toward stillness and presence, changes the biological environment of the immune system.
The work of the UCLA Stress Lab, led by psychoneuroimmunology researcher George Slavich, has consistently shown that social threat, rejection, isolation, and loneliness produce the same proinflammatory cytokine responses as physical threat. The immune system does not distinguish between a predator and a painful breakup at the molecular level. Both activate the same inflammatory cascade. And conversely, genuine social connection and felt safety reduce proinflammatory markers with remarkable consistency.
This is why community is not a luxury in the healing journey. It is biological medicine. It is why the Liberated Life Tribe exists: as a space where the psychoneuroimmunology of human connection can work in your favor rather than against you. Belonging to a community that reflects your wholeness back to you is not just emotionally satisfying. It is immunologically protective.
The mind body connection science here is clear. What you practice, what you feel, what you believe, and who you surround yourself with all send signals that your immune system is reading and responding to at every moment. Once you understand that, wellness stops being a checklist of behaviors and becomes a way of inhabiting your life.
Cytokines, Daily Stress, and the Inflammation Cascade
One of the subtler and more important insights from psychoneuroimmunology is that the stress driving immune dysregulation does not have to be dramatic. It does not have to be a traumatic event, a major loss, or an acute crisis. The research consistently shows that chronic, low grade, ambient stress, the kind that most modern adults consider simply the background texture of their lives, is more than sufficient to elevate proinflammatory cytokines and suppress healthy immune function over time.
Consider the sources of stress that most people normalize as ordinary. Financial anxiety is a persistent neural system activation that many people carry for years without recognizing it as a biological stressor. Relationship tension, even the mild tension of feeling unseen or undervalued, activates the same social threat pathways that psychoneuroimmunology research has linked to proinflammatory cytokine elevation. Digital overwhelm, the constant stream of notifications, comparison, and information overload that defines smartphone existence, activates the threat detection systems of the brain hundreds of times per day without resolution.
Your neural system cannot tell the difference between a threatening email and a physical threat. Both activate CRH. Both trigger the HPA cascade. Both release cortisol. Both affect your immune cells. The difference is that a physical threat is resolved quickly, either you survive or you do not, and the neural system returns to baseline. The email lands in your inbox at 11pm and the unresolved tension of it sits in your body through the night, into the morning, and forward into the next week.
When you multiply that pattern across hundreds of daily micro-stressors over months and years, you get exactly what psychoneuroimmunology predicts: persistently elevated proinflammatory cytokines, suppressed immune surveillance, and a body that is slowly, quietly, continuously tilting toward disease.
A 2025 prospective study of hospital employees, published in Brain Behavior and Immunity Health, found that perceived stress levels consistently preceded declines in wellbeing across measurement periods, with the temporal relationship running from stress to health deterioration rather than the reverse. The study used hair cortisol measurements as an objective biomarker, confirming that the subjective experience of stress maps onto real hormonal changes that affect overall health outcomes.
The good news embedded in all of this is that if low grade, daily, ambient stress is sufficient to drive pathological immune changes, then low grade, daily, ambient joy and regulation are sufficient to reverse them. The levers work in both directions.
Practical Tools to Rewire Your Psychoneuroimmunology Response
This is the part of the psychoneuroimmunology conversation that most wellness writing skips over, leaving you with excellent understanding of the problem and no practical tools for addressing it. That is not how we operate here. Understanding the science without the embodied practice is just anxiety with better vocabulary. So here are the tools that the research in psychoneuroimmunology supports as genuinely effective, explained through the lens of how I actually teach this work.
Breathwork as Neural System Regulation
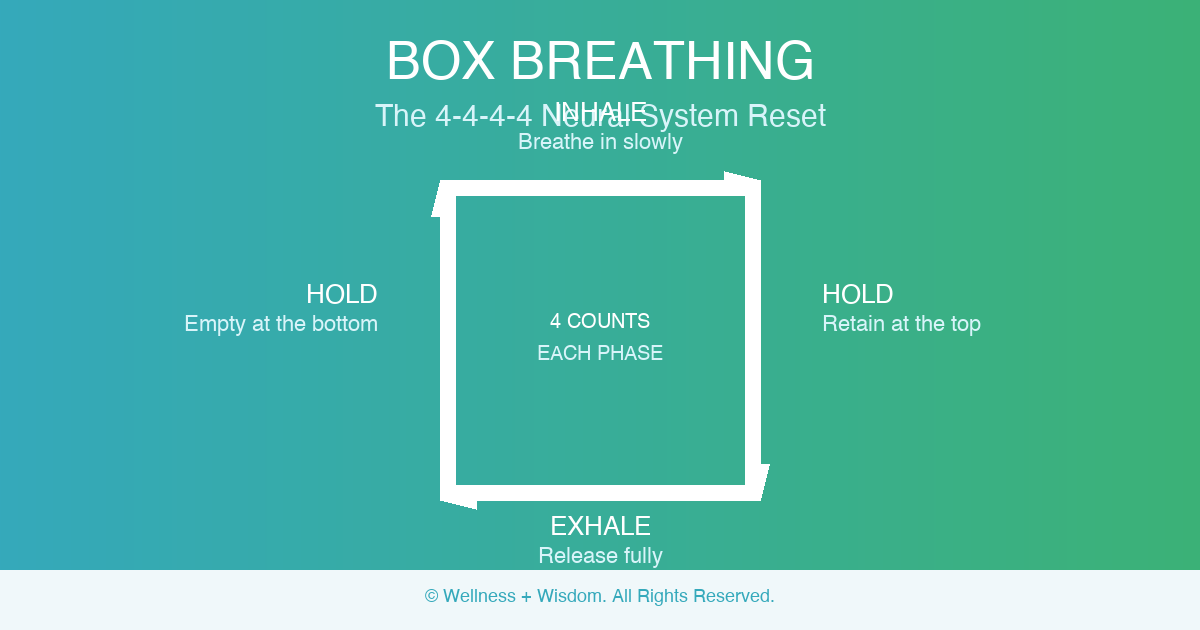
Breathwork is the most direct, evidence-supported intervention in psychoneuroimmunology that most people still underutilize. Here is the core science: breathing is the only physiological function that is both automatic and fully under voluntary conscious control. When you consciously slow and deepen your breathing, you directly activate the parasympathetic branch of the autonomic neural system, reduce cortisol output from the HPA axis, and shift cytokine balance toward a less proinflammatory state.
The breath is the fastest lever you have for changing your internal biochemistry. A simple practice of ten slow, diaphragmatic breaths with an extended exhale can measurably shift your HPA axis response within minutes. This is not a metaphor for calming down. It is a direct biological intervention with documented psychoneuroimmunology effects. The L.I.F.E. Method programs integrate breathwork as a foundational tool precisely because of this direct relationship between breath, neural system state, and immune function.
Completing the Stress Response Cycle
One of the most underappreciated insights from psychoneuroimmunology is that it is not just the experience of stress that drives immune dysregulation. It is the incompletion of the stress response cycle. When a stressor activates your HPA axis and you do not move through a physical resolution of the energy mobilized, the stress hormones, the cytokines, the muscle tension, and the inflammatory signals remain in your body, waiting.
Traditional cultures moved through stress physically: running, fighting, shaking, crying, dancing, and communal grieving. Modern life suppresses most of these. We have the stress activation without the biological completion. Practices that move the body, express emotion, and create felt safety with others (community, connection, physical movement, conscious breathwork) are not indulgences. They are the missing second half of the stress response that psychoneuroimmunology shows you absolutely need.
Community as Immunological Medicine
The work from the UCLA Stress Lab and the broader research base in psychoneuroimmunology is clear: genuine social connection reduces proinflammatory cytokine levels and supports healthy immune function. This is not soft data. Loneliness has been associated with elevated IL-6 levels and increased all-cause mortality with the same statistical force as smoking and obesity.
This is one reason I built the Liberated Life Tribe. Community is not just emotionally supportive. It is biologically protective in the specific ways psychoneuroimmunology identifies as most important: reducing social threat activation, providing coregulation, and creating consistent felt experiences of safety, belonging, and mattering.
Sleep as Epigenetic Immunological Repair
Every hour of restorative sleep is a period of active immune repair and epigenetic recalibration. During sleep, the brain clears inflammatory metabolic waste through the glymphatic system, cytokine balance is restored, cortisol levels fall to baseline, and the immune system conducts surveillance and repair that it cannot perform effectively during waking activation. Chronic sleep deprivation produces the same cytokine profile as chronic stress: elevated IL-6, elevated TNF-alpha, reduced NK cell activity.
Optimizing sleep is not just a wellness recommendation. In the framework of psychoneuroimmunology, it is one of the most powerful daily interventions available for immune function and inflammatory regulation.
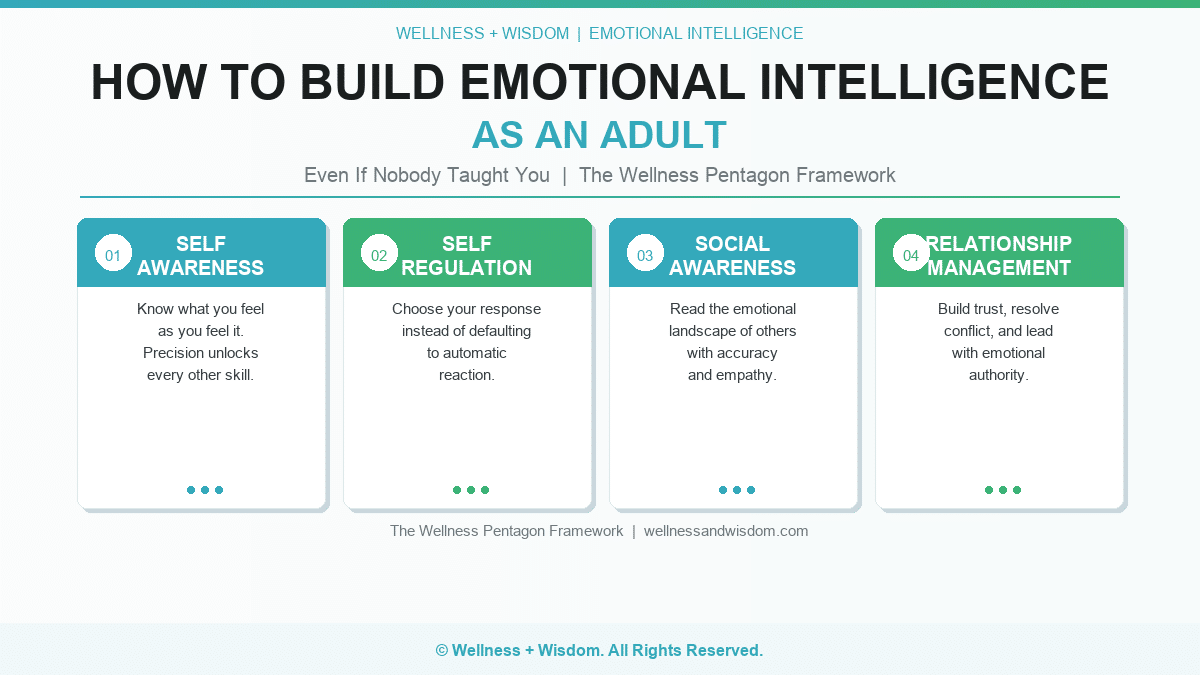
The Wellness Pentagon Applied to Psychoneuroimmunology
The Wellness Pentagon offers a practical framework for addressing all five dimensions of the psychoneuroimmunology environment simultaneously. Physical health (movement, nutrition, sleep) regulates the biological substrate. Mental health (beliefs, cognitive patterns) shapes the perception of threat and safety. Emotional health (feeling and completing the emotional cycle) prevents the chronic unresolved stress states that drive immune dysregulation. Spiritual health (sense of meaning, connection to something larger than the self) has documented antiinflammatory effects in the research. Financial health (resolving financial stressors) addresses one of the most common and persistent ambient stressors in modern life.
Address all five and you are working the full psychoneuroimmunology system. Address only one and you leave four active stressor channels open. This is why integrated, multidimensional approaches to wellness produce better outcomes than single-symptom interventions, and why the science of psychoneuroimmunology points so clearly toward whole-person healing.
For deeper support with this work, explore the programs at Wellness + Wisdom, including the L.I.F.E. Method and the BREATHE program, both designed with the psychoneuroimmunology research specifically in mind. You can also browse the store for additional tools and resources to support your healing journey.
Your Body Wants to Heal: The Good News About Psychoneuroimmunology
Here is the truth that I want you to hold as the foundation underneath everything else in this article: your body's default orientation is toward healing. The stress response, the HPA axis, the cytokine cascade, even the inflammation, these are not malfunctions. They are incredibly sophisticated protective systems doing exactly what they were designed to do. The problem is not that the systems are broken. The problem is that they are activated in environments they were not designed for, without the resolution mechanisms they require.
The field of psychoneuroimmunology is full of evidence not just for how stress causes disease, but for how healing the stress response restores immune function. The body's capacity to shift, adapt, and recover is extraordinary. Neuroplasticity, the brain's ability to rewire its own circuitry, and what researchers are beginning to call immunoplasticity, the immune system's ability to recalibrate when conditions change, are real biological phenomena that operate throughout the entire lifespan.
You are not locked into the stress pattern you inherited. You are not condemned to the proinflammatory state that years of chronic stress may have established. The science of psychoneuroimmunology does not offer a grim verdict. It offers a precise map of the mechanisms you can work with to shift the trajectory of your health, starting now, with the choices available to you today.
The latest research from the Wellness + Wisdom Podcast conversations and from peer reviewed journals converges on the same insight: joy, genuine felt joy, not the performance of positivity, but the real experience of safety, connection, meaning, and aliveness, is an epigenetic signal. It has a measurable antiinflammatory effect. It is medicine for the immune system at the molecular level.
This is the core invitation of Emotional Epigenetics: you are not bio-energetically doomed. You are bio-energetically burdened with patterns that are, with the right understanding and the right practices, completely addressable. And when you address them, you are not just healing yourself. You are changing what you pass forward to your children for seven generations and beyond.
That is the promise and the possibility that psychoneuroimmunology makes visible. The path from sick to well runs through the same doorway as the path from fearful to free: the body, the breath, the community, and the courageous willingness to feel, process, and move through what has been stored. That path is available to you. It is available right now.
Frequently Asked Questions About Psychoneuroimmunology
What is psychoneuroimmunology in simple terms?
Psychoneuroimmunology is the scientific study of how the mind, the neural system, and the immune system communicate with each other. In simple terms, it is the formal science of the mind body connection. It shows that your thoughts, emotions, and stress levels send biological signals that directly affect how your immune system works, and that your immune system sends signals back that affect your mood, energy, and mental state. It is a two way biological conversation that never stops.
How does stress affect the immune system according to psychoneuroimmunology?
According to psychoneuroimmunology, stress affects the immune system through several interconnected pathways. The most important is the HPA axis, which causes the adrenal glands to release cortisol in response to perceived threat. In the short term, cortisol regulates and modulates immune activity appropriately. But with chronic stress, cortisol becomes dysregulated, glucocorticoid receptor resistance develops, and proinflammatory cytokines like IL-6 and TNF-alpha begin to circulate persistently. The net effect is suppressed immune surveillance (making you more susceptible to infection) alongside elevated systemic inflammation (contributing to chronic disease). Peer reviewed studies including the 1991 NEJM Cohen study have documented these effects directly in human subjects.
Can psychoneuroimmunology explain autoimmune disease?
Psychoneuroimmunology offers important mechanistic insights into autoimmune disease, though it does not claim to be a complete explanation for any single condition. The research shows that chronic stress and HPA axis dysregulation create an immunological environment characterized by cytokine imbalance, reduced immune regulation, and shifts toward proinflammatory activity. This is the same biological environment associated with autoimmune flares and potentially autoimmune initiation. A 2025 review published on PubMed (PMID 41155288) specifically documented the connections between chronic stress, cortisol dysregulation, and conditions including lupus, rheumatoid arthritis, and multiple sclerosis. This does not mean stress alone causes autoimmune disease, but it is a significant and often underappreciated contributing factor in the current evidence.
What does mind body connection science tell us about healing?
Mind body connection science, including the field of psychoneuroimmunology, tells us that healing is not exclusively physical. The biological state of your immune system is continuously shaped by your psychological experience, emotional patterns, social relationships, and sense of safety. This means that therapeutic practices that address these dimensions, including breathwork, community, meditation, emotional processing, and embodied movement, are not complementary luxuries sitting alongside real medicine. They are direct interventions in the biological systems that determine immune health. The research on breathwork, meditation, and social connection all shows measurable antiinflammatory and immune-supportive effects consistent with what psychoneuroimmunology predicts.
How can I start using psychoneuroimmunology principles in my daily life?
The most accessible entry points into applying psychoneuroimmunology in daily life are breathwork, genuine community connection, sleep optimization, and stress completion practices. Breathwork directly regulates the HPA axis and shifts cytokine balance within minutes. Community connection reduces social threat activation, which the research identifies as a major proinflammatory driver. Sleep gives your immune system the daily repair window it needs. Stress completion practices, physical movement, emotional expression, and breath work, allow the stress response cycle to resolve rather than accumulate. Beyond these fundamentals, working with a framework like the L.I.F.E. Method provides structured support for addressing the emotional and belief-based roots of chronic stress activation, which is where psychoneuroimmunology says much of the immune dysregulation originates.
Is psychoneuroimmunology recognized by mainstream medicine?
Psychoneuroimmunology is a recognized and active scientific discipline with its own professional society (the Psychoneuroimmunology Research Society), its own peer reviewed journals, and thousands of published studies in mainstream biomedical publications including the New England Journal of Medicine, Nature, and leading immunology and psychiatry journals. The research base is robust and growing. However, because medical specialization tends to organize the body into separate departments, the field has not yet been systematically integrated into standard clinical training. This is changing, particularly in the fields of integrative medicine, psychosomatic medicine, and health psychology. If your doctor has not mentioned it, that does not mean the science is not valid. It means the field is ahead of standard curriculum adoption.
Ready to Put This Science Into Practice?
The best understanding of psychoneuroimmunology in the world is worth nothing without the community, the tools, and the embodied practices to use it. That is what the Liberated Life Tribe exists for. Join us and receive the free 10 day Self Liberation Blueprint, a guided journey through the exact practices that the science of psychoneuroimmunology says move the needle on your immune health, your stress response, and your capacity for authentic joy.
Join the Liberated Life Tribe and Receive Your Free 10 Day Self Liberation Blueprint
Free to join. No credit card required. Available at liberatedlife.com
Explore the Liberated Life Tribe community at Wellness + Wisdom →
This article is for educational purposes only. It does not constitute medical advice. If you have concerns about your immune health or chronic disease, please consult a qualified healthcare professional.